An acoustic neuroma, also known as vestibular schwannoma, is a slow-growing, non-cancerous tumour that develops on the vestibular nerve, which connects your inner ear to your brain. This nerve transmits sound and balance information from your ear to your brain. The tumour originates from Schwann cells (cells that wrap around nerve fibres) and typically grows slowly, though growth rates vary between individuals. Acoustic neuromas are a type of intracranial tumour, with cases commonly diagnosed in adults between 40 and 60 years of age.
Acoustic Neuroma in Singapore
If you’ve been experiencing hearing loss in one ear, persistent ringing sounds, or unexplained balance problems, you may be dealing with an acoustic neuroma. While discovering a brain tumour can be concerning, acoustic neuromas are benign (non-cancerous) growths that can be managed with contemporary treatment approaches. At our clinic, our ENT Specialist provides comprehensive evaluation and treatment for acoustic neuroma, utilising modern diagnostic techniques and evidence-based treatment protocols that aim to preserve your hearing and quality of life whenever possible. Individual results and timelines may vary.

Dr Gan Eng Cern
MBBS
MRCS (Edin)
mmed (orl)
FAMS
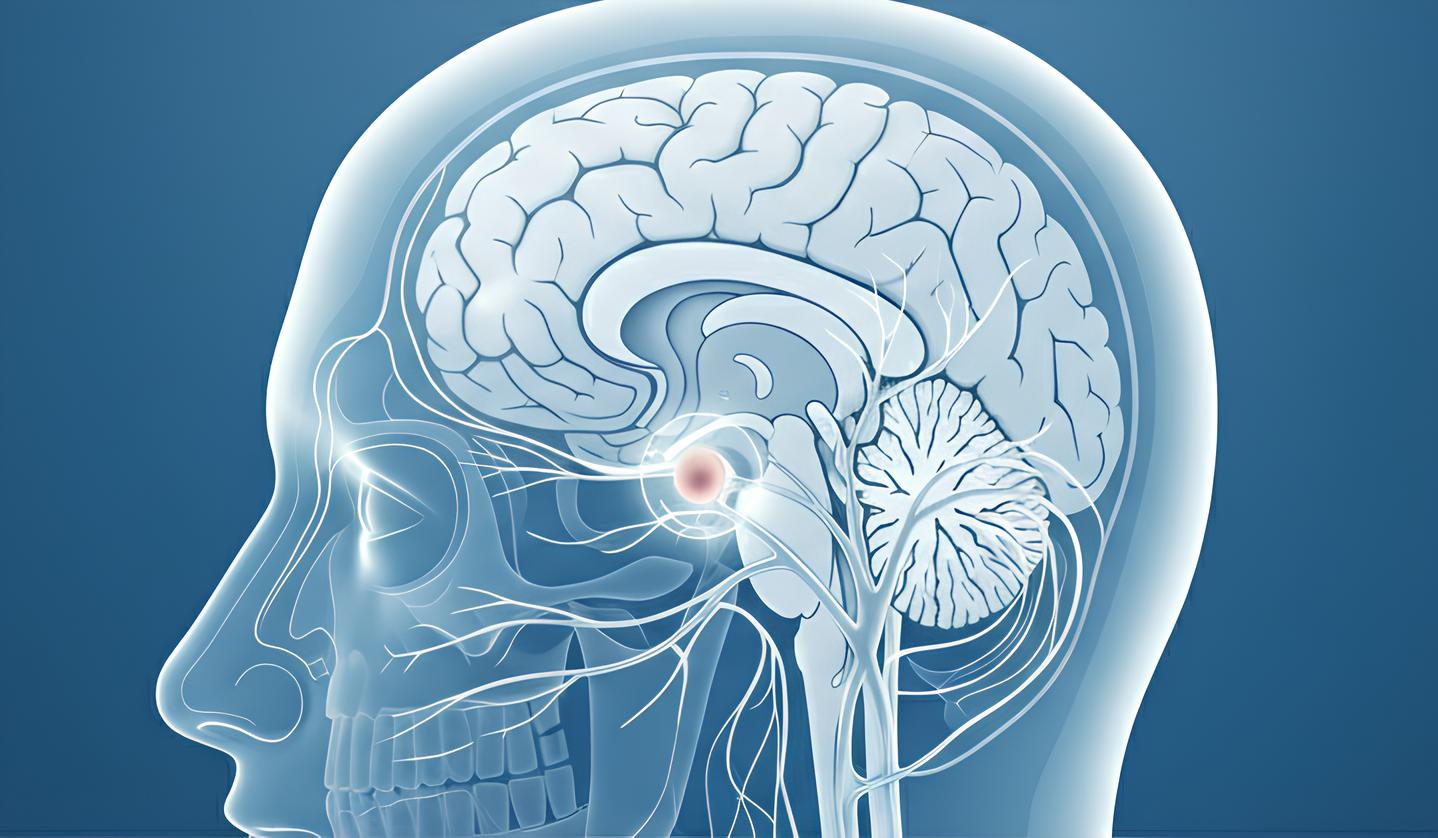

What is Acoustic Neuroma?
Types of Acoustic Neuroma
- Sporadic Acoustic Neuroma: This is the most common form. Sporadic acoustic neuromas typically occur on one side only (unilateral) and develop without any known genetic cause. These tumours usually appear in middle-aged adults and grow slowly over many years.
- Neurofibromatosis Type 2 (NF2) Related: This inherited form is less common. Patients with NF2 often develop acoustic neuromas on both sides (bilateral) and may present at a younger age, sometimes in their teens or twenties. NF2-related tumours tend to grow more aggressively and require specialised management approaches.
- Intracanalicular Acoustic Neuroma: These tumours remain confined within the internal auditory canal, the bony channel through which the vestibulocochlear nerve passes. They tend to be smaller and may cause symptoms earlier due to the confined space.
- Extracanalicular Acoustic Neuroma: These larger tumours extend beyond the internal auditory canal into the cerebellopontine angle (the space between the cerebellum and pons in the brain). They can compress surrounding structures including the brainstem and other cranial nerves.
Causes & Risk Factors
Causes
The exact cause of sporadic acoustic neuromas remains unknown. Current research suggests that these tumours may arise from genetic mutations in the Schwann cells of the vestibular nerve. The NF2 gene, located on chromosome 22, produces a protein called merlin or schwannomin that normally helps regulate cell growth. When this gene is mutated or absent, uncontrolled cell growth can occur, which may lead to tumour formation.
Risk Factors
- Genetic predisposition: Having NF2 may increase risk, with acoustic neuromas being associated with NF2 patients
- Age: Most commonly occurs in middle-aged adults, though can occur at any age
- Previous radiation exposure: High-dose radiation to the head, particularly during childhood, may increase risk
- Mobile phone use: While extensively studied, current evidence does not establish a definitive link
- Family history: Having a parent with NF2 may increase the chance of inheriting the condition
- Loud noise exposure: No proven association, despite affecting the same nerve
Signs & Symptoms
Early Symptoms
- Gradual hearing loss in one ear
- Tinnitus (ringing, buzzing, or roaring sounds in the affected ear)
- Feeling of fullness or pressure in the ear
- Subtle balance disturbances when turning quickly
- Occasional mild dizziness
Progressive Symptoms
- Worsening hearing loss, potentially leading to complete deafness in affected ear
- Persistent unsteadiness or vertigo episodes
- Difficulty understanding speech, especially in noisy environments
- Facial numbness or tingling (affecting cranial nerve V)
- Difficulty swallowing or hoarseness (rare, affecting cranial nerves IX and X)
- Headaches, particularly in the morning
Advanced Symptoms
- Complete hearing loss in the affected ear
- Severe balance problems affecting daily activities
- Facial weakness or paralysis (affecting cranial nerve VII)
- Double vision or other visual disturbances
- Hydrocephalus symptoms (confusion, gait problems, urinary incontinence)
- Signs of brainstem compression
Symptoms typically develop gradually over months to years, though sudden hearing loss can occasionally occur due to tumour-related vascular changes or inner ear fluid alterations. The progression and severity of symptoms may vary with tumour size and growth rate.
Experiencing these symptoms? Consider seeking medical evaluation.
Consult with an ENT specialist for proper assessment and treatment options.

When to See an ENT Specialist
Seek immediate medical attention if you experience sudden hearing loss in one ear, as this requires urgent evaluation and potential treatment within 72 hours. Progressive hearing loss in one ear, persistent tinnitus lasting more than two weeks, or unexplained balance problems also warrant prompt consultation with an ENT specialist in Singapore. Red flag symptoms requiring immediate assessment include facial weakness or paralysis, severe persistent headaches with morning vomiting, vision changes, or difficulty walking.
During your first consultation, an ENT specialist in Singapore will conduct a thorough medical history review, focusing on your symptoms’ onset, progression, and impact on daily life. The examination includes otoscopy (ear examination), hearing tests, and neurological assessment of cranial nerve function. Early diagnosis is important as smaller tumours may offer more treatment options and potentially better outcomes for hearing preservation. Delaying treatment may result in irreversible hearing loss and increased surgical complexity if intervention becomes necessary.


Diagnosis & Testing Methods
- Audiometry Testing: Comprehensive hearing assessment is the first diagnostic step. Pure tone audiometry measures hearing thresholds across different frequencies, typically showing asymmetric sensorineural hearing loss. Speech audiometry evaluates word recognition scores, which may be disproportionately affected compared to pure tone results in acoustic neuroma patients. These tests require no special preparation.
- Magnetic Resonance Imaging (MRI): MRI with gadolinium contrast is considered a standard diagnostic approach for acoustic neuromas. This imaging can detect small tumours and provides detailed information about tumour size, location, and relationship to surrounding structures. Patients with claustrophobia may request mild sedation.
- Auditory Brainstem Response (ABR): This test measures electrical activity in the auditory nerve and brainstem in response to sound stimuli. ABR can detect retrocochlear pathology (problems beyond the inner ear) and helps differentiate acoustic neuroma from other causes of hearing loss. The test is non-invasive and requires the patient to remain still and relaxed.
- Vestibular Testing: Videonystagmography (VNG) or electronystagmography (ENG) assesses balance function by measuring eye movements in response to various stimuli. Caloric testing evaluates each ear’s vestibular response independently. These tests help determine the extent of vestibular nerve involvement and may assist in treatment planning. Patients should avoid certain medications before testing as advised by their healthcare provider.
Treatment Options Overview
Observation (Watch and Wait)
For small tumours with minimal symptoms, especially in older patients, active surveillance may be appropriate. This involves regular MRI scans and hearing monitoring with audiometry. Treatment is initiated if growth or symptom progression occurs.
Stereotactic Radiosurgery
This non-invasive treatment delivers precisely focused radiation to the tumour in a single session (Gamma Knife) or multiple sessions (fractionated stereotactic radiotherapy). Suitable for certain tumour sizes, radiosurgery aims to stop tumour growth rather than remove it. Treatment duration varies, requires no incision, and patients typically return home the same day.
Microsurgical Removal
Surgical excision may be recommended for larger tumours, growing tumours, or those causing symptoms. Three main surgical approaches exist, each chosen based on tumour characteristics and hearing status. The procedure is performed under general anaesthesia. Modern techniques including intraoperative neurophysiological monitoring help preserve facial nerve function.
Middle Fossa Approach
This approach accesses the tumour through a window in the temporal bone above the ear. It’s suitable for small intracanalicular tumours when hearing preservation is attempted. The approach provides visualisation of the internal auditory canal but is limited for larger tumours extending into the cerebellopontine angle.
Translabyrinthine Approach
This approach goes through the mastoid bone and inner ear structures, sacrificing hearing but providing facial nerve visualisation. It’s preferred for patients with non-serviceable hearing or large tumours where hearing preservation is not feasible. This approach may offer reduced risk of cerebrospinal fluid leak.
Retrosigmoid/Suboccipital Approach
This approach accesses the tumour through an opening behind the ear, preserving inner ear structures. It’s suitable for tumours of various sizes when hearing preservation is attempted. This versatile approach allows removal of large tumours but may carry a risk of post-operative headaches compared to other approaches.
Every patient’s condition is unique.
Our ENT specialist will assess your specific situation and recommend the most suitable treatment approach for you.

Complications if Left Untreated
Without treatment, acoustic neuromas may continue growing, though growth rates vary considerably between individuals. Progressive enlargement can lead to hearing loss in the affected ear, which may become irreversible once the cochlear nerve is damaged. Balance problems may worsen, potentially affecting mobility and increasing fall risk.
Large untreated tumours can compress the facial nerve, potentially causing facial weakness or paralysis that may affect eating, drinking, and eye closure. Brainstem compression from large tumours can potentially disrupt vital functions including breathing, heart rate, and blood pressure regulation. Hydrocephalus (fluid buildup in the brain) may develop when tumours obstruct normal cerebrospinal fluid flow, potentially causing confusion, gait disturbances, and urinary incontinence. In some cases, large tumours can become serious, though this may be preventable with appropriate monitoring and timely intervention. Individual outcomes and progression rates may vary considerably between patients.
Medisave & Insurance Shield Plan approved
Your ENT procedure may be eligible for Medisave claims, with the claimable amount varying based on the procedure’s complexity. For additional options, including the use of your insurance or Integrated Shield Plan, reach out to our friendly clinic staff today for assistance.
Frequently Asked Questions (FAQ)
Can acoustic neuromas become cancerous or spread to other parts of the body?
No, acoustic neuromas are benign tumours that do not become cancerous or spread to other body parts. They remain localised to the vestibular nerve area, though they can grow and compress nearby structures. While non-cancerous, their location near important brain structures means they still require appropriate monitoring or treatment to prevent complications from local growth and compression effects.
What are the chances of preserving my hearing with treatment?
Hearing preservation depends on several factors including tumour size, location, current hearing level, and treatment choice. The likelihood of hearing preservation varies with different treatment approaches. Observation may help maintain hearing in slow-growing tumours. Our ENT Specialist will assess your specific situation and discuss realistic expectations based on your tumour characteristics and chosen treatment approach.
How long is the recovery period after acoustic neuroma surgery?
Hospital stay typically involves several days following surgery, depending on the surgical approach and individual recovery. Initial recovery at home may take several weeks, during which you’ll gradually increase activity levels. Return to work and activities varies by individual circumstances. Balance rehabilitation often continues as your brain adapts to changes in vestibular input. Recovery is highly individual, with various factors affecting the timeline.
Will I need hearing aids or other devices after treatment?
If hearing is affected in the treated ear, several rehabilitative options exist. Conventional hearing aids may help if some hearing remains. For single-sided deafness, CROS (Contralateral Routing of Signal) hearing aids can transmit sound from the affected ear to the hearing ear. Bone-anchored hearing devices (BAHA) use bone conduction to transmit sound. Your audiologist will recommend appropriate devices based on your specific hearing status and lifestyle needs.
What follow-up care is required after treatment?
Long-term monitoring is essential regardless of treatment choice. After surgery or radiation, MRI scans may be performed at regular intervals. Hearing tests may be conducted if hearing is preserved. After radiation therapy, temporary tumour changes may occur, requiring monitoring. For observed tumours, MRI frequency depends on individual circumstances and growth patterns.
Can acoustic neuromas recur after treatment?
Treatment outcomes vary depending on the approach used. Complete surgical removal aims for low recurrence rates. Partial removal may have different recurrence considerations. After radiation therapy, tumour control can be achieved in many cases, though some patients may require additional treatment. Regular monitoring with MRI helps detect any changes, allowing prompt intervention if needed.
Conclusion
Acoustic neuroma, whilst being a benign tumour, requires careful evaluation and management due to its location near critical structures controlling hearing, balance, and facial function. Modern treatment options including observation, stereotactic radiosurgery, and microsurgical techniques may offer outcomes when appropriately selected based on tumour characteristics and patient factors. Early diagnosis may help with preserving hearing and minimising treatment complexity. With proper management and monitoring, patients with acoustic neuroma may maintain quality of life and functional outcomes.
Take the First Step Towards Better Health
Living with acoustic neuroma can be challenging, but you don’t have to face it alone. Our ENT Specialist has experience diagnosing and treating acoustic neuroma using evidence-based approaches.


Dr Gan Eng Cern
MBBS
MRCS (Edin)
mmed (orl)
FAMS
With over 15 years of experience, Dr Gan specialises in the comprehensive management of a broad range of conditions related to the ear, nose and throat (ENT), and head and neck.
Dr. Gan has contributed to the academic field as a Senior Clinical Lecturer at the Yong Loo Lin School of Medicine, National University of Singapore. He underwent his subspecialty training in Rhinology (Nose & Sinus conditions) and Endoscopic Skull Base Surgery at the renowned St Paul’s Sinus Center, part of the University of British Columbia in Vancouver, Canada. He is recognised for his extensive research work, with numerous contributions to reputable international ENT journals. Dr Gan is also highly sought after as a speaker and has shared his surgical knowledge as a surgical dissection teacher at various prominent ENT conferences and courses.
- 2020 – Reader’s Choice Gold Award for Best ENT Specialist (Expat Living Singapore)
- 2016 – Best Educator Award (Eastern Health Alliance)
- 2016 – “Wow” Award (Patient Compliment)
- 2014 – Eastern Health Alliance Caring Award – Silver
- 2014 – 19th Yahya Cohen Memorial Lectureship (awarded by the College of Surgeons, Academy of Medicine Singapore for best scientific surgical paper)
- 2012 – Human Manpower Development Award (Ministry of Health, Singapore)
- 2007 – Singhealth Best Doctor Award
Qualifications
- MBBS – Bachelor of Science, Bachelor of Medicine, Bachelor of Surgery (University of New South Wales, Sydney, Australia)
- MRCS (Edin) – Member of the Royal College of Surgeons Edinburgh, United Kingdom
- MMed (ORL) – Master of Medicine in ENT (National University of Singapore)
- FAMS – Fellow of the Academy of Medicine Singapore

Make an Enquiry
Fill up the form and our friendly clinic staff will get back to you promptly.
Our Location
A Specialist Clinic for Sinus, Snoring & ENT
38 Irrawaddy Road #08-45
Mount Elizabeth Novena Hospital
Singapore 329563
Mon – Fri: 9:00 am – 5:00 pm
Sat: 8:30 am – 12:00 pm
