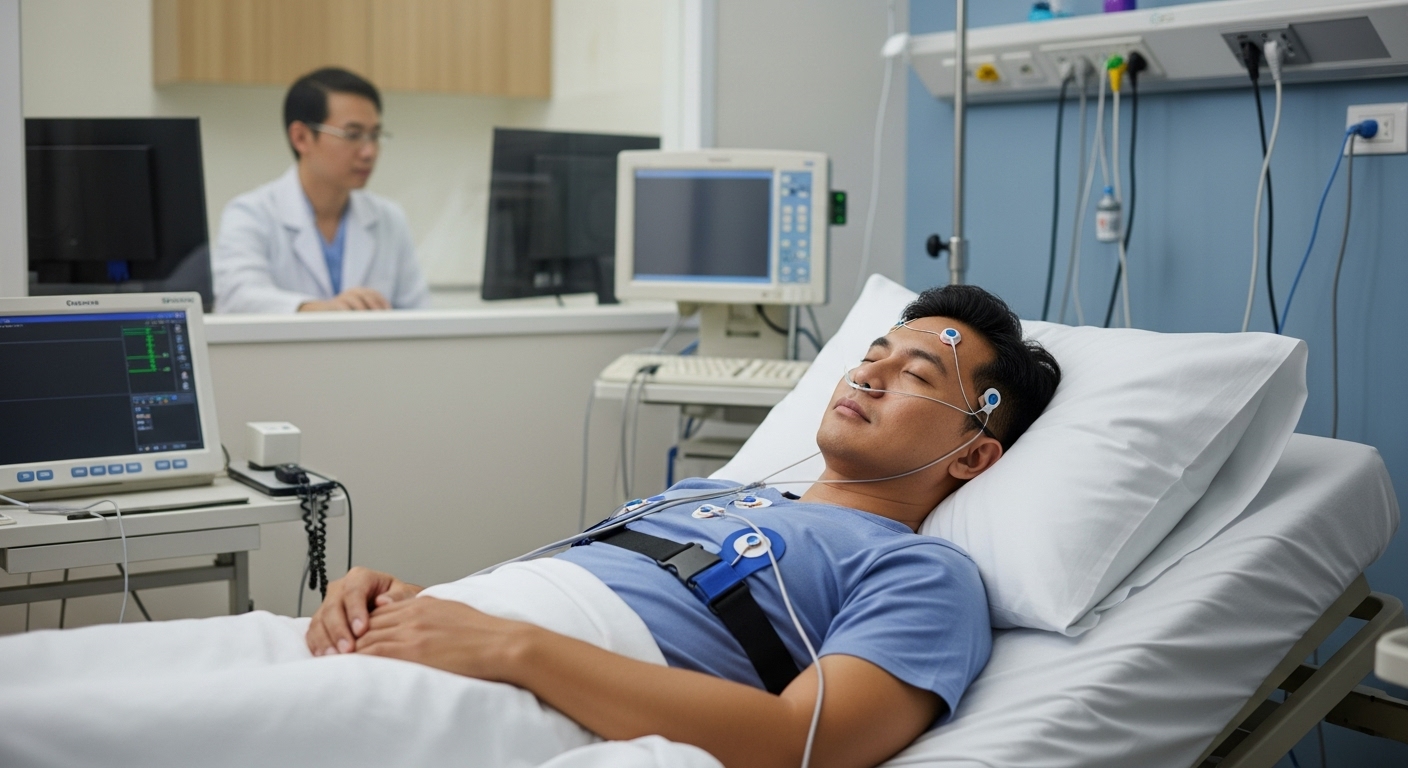
A sleep study, or polysomnography, is a non-invasive diagnostic test that records multiple body functions while you sleep. This evaluation monitors brain waves (EEG), eye movements (EOG), muscle activity (EMG), heart rhythm (ECG), breathing patterns, oxygen levels, and body movements throughout the night. The study captures data about your sleep stages, breathing interruptions, and any abnormal movements or behaviours during sleep.
Sleep studies are used to diagnose sleep-related breathing disorders, particularly obstructive sleep apnoea (OSA), where the airway repeatedly becomes blocked during sleep. The test also identifies central sleep apnoea, where the brain temporarily stops sending signals to breathe, and complex sleep apnoea syndrome. Beyond breathing disorders, sleep studies can diagnose periodic limb movement disorder, narcolepsy, REM sleep behaviour disorder, and unexplained chronic insomnia. The data collected may help an ENT specialist understand your condition and develop an appropriate treatment plan.