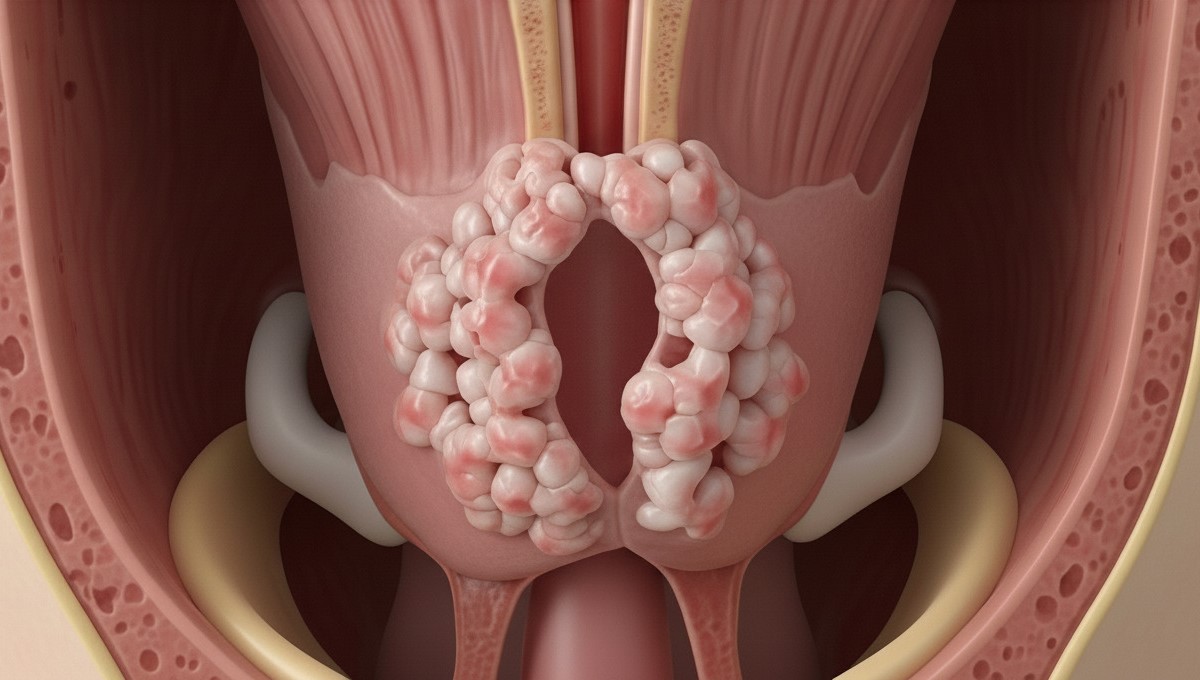
Accurate diagnosis of oropharyngeal cancer requires a systematic approach combining clinical examination with diagnostic procedures. The initial evaluation begins with a comprehensive physical examination of your mouth, throat, and neck. An ENT specialist uses specialised mirrors and lights to examine hard-to-see areas of your oropharynx.
Flexible nasopharyngoscopy allows detailed visualisation of your throat using a thin, flexible tube with a camera. This procedure is performed in the clinic with local anaesthetic spray and provides visual assessment of any abnormal areas.
If suspicious areas are identified, a biopsy may be recommended for definitive diagnosis. This may be performed in the clinic under local anaesthesia for accessible lesions, or under general anaesthesia for deeper areas. Tissue samples are examined by pathologists to confirm the presence and type of cancer cells.
Imaging studies play a role in staging the cancer. CT scans provide detailed images of the primary tumour and neck lymph nodes. MRI scans offer soft tissue detail and can be useful for assessing tongue base tumours. PET-CT scans help detect distant spread and are used for treatment planning.
HPV testing on biopsy samples has become standard practice, as HPV status can influence treatment decisions and prognosis. Individual results and timelines may vary. This information is provided for educational purposes and does not replace consultation with a healthcare professional.